
Minimally invasive surgery in modern gynaecology
By Dr Simon SEE Emvula.
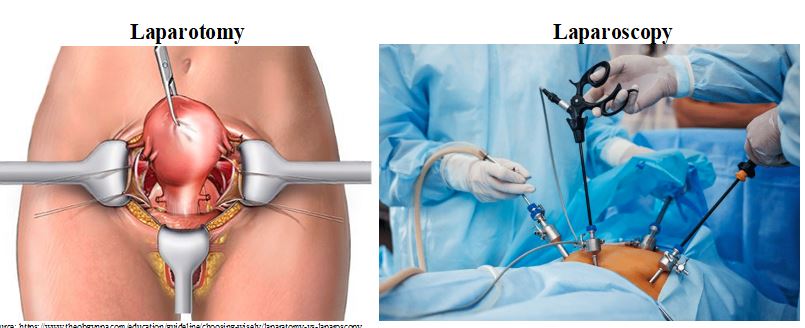
Minimally invasive surgery can be considered the greatest surgical innovation. This innovation brought a change to the traditional surgical approach (known as laparotomy) of making a large incision on the skin to enter the abdominal cavity without affecting the surgical results and safety.
Minimally invasive surgical techniques are performed with a digital camera connected to a telescope that is inserted either into the abdomen (known as a laparoscopy) or through the cervix into the uterine cavity(known as hysteroscopy).
The camera provides the surgeon with a clear view of the procedure, which is projected on high definition digital video monitors. Operating instruments are inserted through the small incisions to avoid making a large incision on the abdominal wall. It is well established that minimally invasive surgery leads to decreased length of hospital stay, improved patient outcomes, and increased patient satisfaction compared to open abdominal gynaecologic surgery.
Other advantages over conventional surgery are less pain, less blood loss, smaller incisions, less risk of infection and faster recovery. Additionally, the smaller incisions result in better cosmetic results and minimal scarring. The field of gynaecologic surgery is clearly not an exemption as minimally invasive gynaecological surgery has gained momentum within the speciality.
Minimal invasive surgery can diagnose and manage most gynaecological conditions. Common gynaecological procedures performed by laparoscopy include, but are not limited to sterilization (tubal ligation), myomectomy (uterine fibroid removal), deep endometriosis, infertility procedures, ovarian cysts removal (non-cancerous), managing ectopic pregnancies, ovarian torsion and hysterectomy (removal of the womb). Minimally invasive procedures can be performed as day procedures meaning patients return home on the same day of the surgery depending on the magnitude of the procedure. Considering that patients recover faster and return to work earlier compared to conventional surgery, minimally invasive surgery has the potential to be of high economic value. Hysteroscopy allows the surgeon to assess the uterine cavity and perform procedures such as myomectomy.
Operative vaginal procedures are considered minimally invasive since no surgical incisions are made on the skin. A vaginal hysterectomy (removal of the womb through the vagina) is the first well-published known minimally invasive gynaecological surgical procedure.
However, this procedure although relatively safe in good hands is limited by poor visualization of the surgical operation field.
Despite all the benefits of minimally invasive surgery over traditional open surgery; not all patients qualify for minimally invasive surgery due to specific gynaecological conditions that will make it unsuitable for them. In such cases, traditional open surgery will be recommended; therefore it is important to discuss the modes of surgery with your gynaecologist so that one can make an informed decision.
Minimally invasive surgery is considered to be the standard mode of surgery in modern gynaecology. Looking into the future, robotic-assisted gynaecological surgery has been making strides over the past few years and will surely become the mode of choice in gynaecological surgery in the near future.












































